Chronic Pelvic Pain
Chronic pelvic pain is common condition that can affect up to 1/3 of women and accounts for 20% of visits to Gynecologists. Unfortunately, routine tests will not identify a source of pain in up to 30% of patients. Pelvic varices (also known as “pelvic venous disorder”) accounts for up to 16-31% of patients with chronic pelvic pain without an alternative diagnosis.
Pelvic Venous Disease
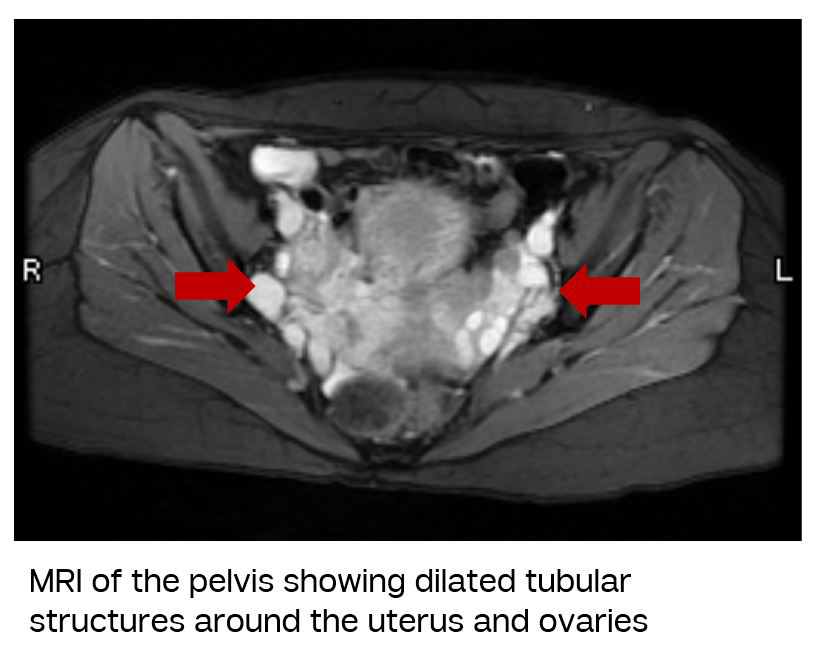
Pelvic Venous Disorder occurs because dilated veins (also known as varices) in the pelvis irritate nerves in the pelvis leading to symptoms of cramping, heaviness or discomfort. These veins can also lead to vulvar varicose veins or thigh varicose veins. The symptoms are typically worse with:
- Prolonged standing
- Prolonged sitting
- During or for an extended time following intercourse
- During or following menstrual cycles
What is the Cause of Pelvic Venous Disease
Pelvic varices (dilated veins) are similar to varicose veins in the legs and are due to increased pressure in the veins. The most common reason for increased pressure in the veins around the uterus and ovaries are poorly functioning valves in the veins that lead to excess blood leaking into the pelvic veins. A blockage of blood flow out of the pelvis can also lead to dilated veins in the pelvis.
Diagnosis
Women will typically have seen several physicians to exclude other diagnoses that can cause pelvic pain. You will be evaluated by one of our physicians specializing in abnormal pelvic veins, which includes a review of prior assessments by other physicians and imaging review, after which you may be sent for an MRI or an ultrasound to identify the reason for your pelvic varices and help plan appropriate treatment.
Treatment Options
Once the cause for the pelvic varices is identified, we will discuss the best treatment option. If the cause is “leaking” veins, then the treatment may include closure (aka embolization) of the abnormal vein. If the cause is a blockage of a vein, then the treatment may include placement of a stent to open the blocked vein segment.

